Immune Cells Can 'Smell' Their Environment
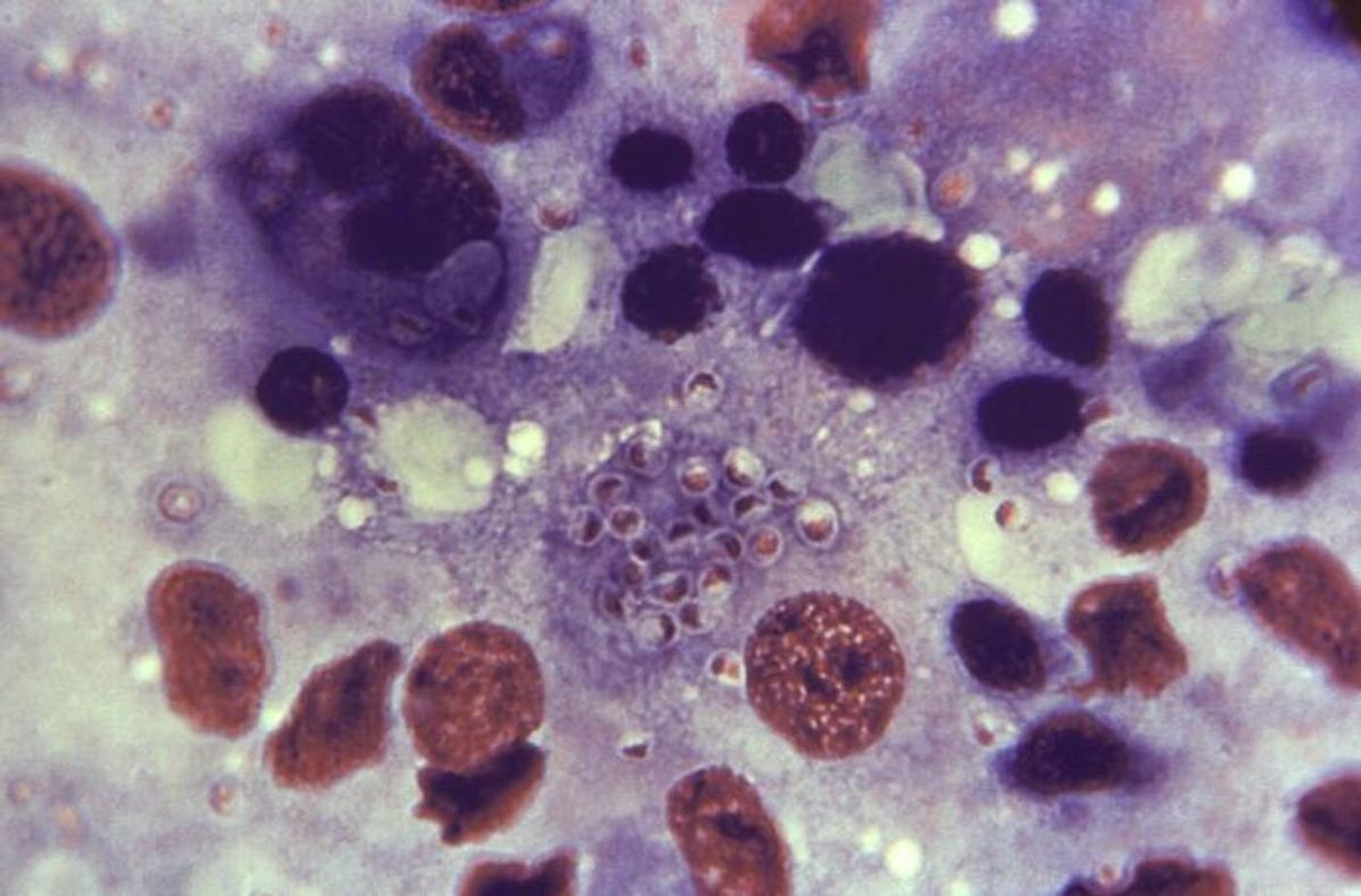
Immune cells called macrophages are on the front lines of our body's defense system; macrophages can detect pathogens and fight against them. Researchers have found that macrophages can 'sniff out' their targets, and now, scientists have shown how that can trigger inflammation. Macrophages in the vascular system have been found to possess olfactory receptors, which are best known for enabling us to smell stuff. But for macrophages, these receptors are one way to identify harmful invaders and promote an immune response. But too much inflammation can be dangerous, and when olfactory receptors on macrophages are overstimulated, they may cause atherosclerosis, which can lead to blood clots or heart problems. The findings have been reported in Science.
In 2019, scientists showed that some macrophages that sit in the walls of blood vessels carry olfactory receptors. Additional research indicated that the immune cells use an olfactory receptor called OR6A2 to sense a molecule called octanal. This latest study has shown that octantal is present in the blood of humans and mice at low levels, but there is enough to activate OR6A2. High levels of octanal have been associated with higher biomarkers of cardiovascular disease. When OR6A2 on macrophages binds to octanal, the NLRP3 inflammasome is activated, and interleukin-1β is released from human and mouse macrophages.
In this study, the researchers showed that when octanal was detected, it promoted arterial inflammation. The investigators injected two groups of mice with octanal, one group was normal and the other group of mice was engineered to lack the gene Olfr2 (olfactory receptor 2), which encodes for OR6A2, the olfactory receptor for octanal. In the mice that could detect octanal, atherosclerotic plaques formed.
When the researchers blocked the ocatanal-detecting olfactory receptor with a molecule called citral, the inflammation was reduced; if macrophages could not sense octanal, the atherosclerosis was reversed.
Additional work will be needed to show that this mechanism is at work in people as well, but the researchers are hopeful that this study will lead to new therapeutics.
Now, the scientists also want to learn more about other olfactory receptors that macrophages carry, and how they work in humans.
“This study is just the first hint of something new. It’s opened up years of research ahead of us,” said first study author Marco Orecchioni, Ph.D., an instructor at the La Jolla Institute for Immunology.
Sources: La Jolla Institute for Immunology, Science