The Origins of Hospital Acquired Infections - Do They Come From the Patient?
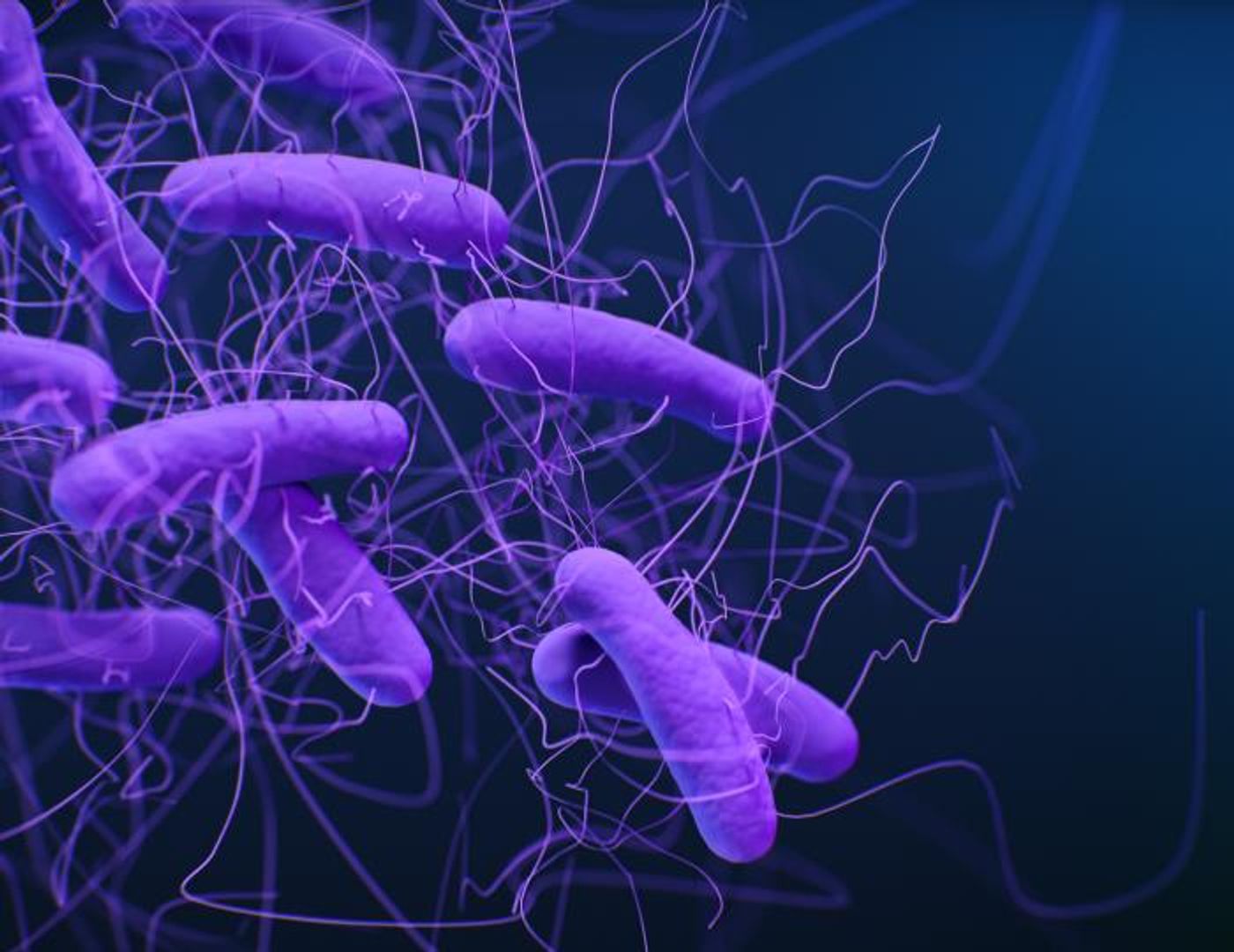
Hospitals are supposed to help sick people get healthy, but unfortunately, many hospitalized patients become sick with infection during their stay. There have been major efforts to reduce the number of infections that are acquired in hospitals, and there have been some reductions. But about 3.2 percent of those hospitalized in the US, 6.5 percent in the European Union get an infection in the hospital. Clostridioides difficile (C. diff) is the primary bacterial cause of healthcare-associated infections in the United States.
Like many bacteria, C. diff can be carried harmlessly by people. But this is a microbe that can take advantage of opportune times, like when people are sick, or their immune systems are weakened to cause infection. C. diff is estimated to cause around half a million infections in the US alone every year. Scientists have now found that many of those infections are coming from within the patients. The findings have been reported in Nature Medicine.
In this study, the researchers analyzed infections in about 1,100 people who had been patients in the intensive care unit at Rush University Medical Center over a period of nine months. They determined that around 9 percent carried C. diff bacteria. Whole genome sequencing was then applied to 425 strains of C. diff that had been isolated from almost 4,000 fecal samples. The bacterial genomes were then compared to reveal more about how they were spreading.
"By systematically culturing every patient, we thought we could understand how transmission was happening. The surprise was that, based on the genomics, there was very little transmission," said study co-leader Evan Snitkin, PhD of the University of Michigan Medical School.
The strains were not alike, which suggested that these patients were not getting the infection from one another in the hospital. During the nine-month study, there were only six cases in which there was evidence of transmission of a strain from one patient to another. It was individuals who were already carrying C diff before they came to the hospital who were experiencing infections while staying there.
More work will be needed to understand what triggered a change in C. diff to cause symptoms of infection in patients like diarrhea and cramping.
Study co-leader Mary Hayden, MD, of Rush University Medical Center, noted that strategies used by hospitals to prevent infection, like frequent handwashing among personnel, and routine disinfection of rooms with an antibacterial that kills C. diff, are still necessary. The low rate of patient-to-patient transmission may very well be due to these measures. This work has shown, however, that more efforts will be needed to understand why these infections emerge and how to prevent them.
C. diff is everywhere in the environment, and we can't eradicate it. These bugs are also resistant to alcohol-based hand sanitizer, added study co-leader Vincent Young, MD, PhD, of the University of Michigan Medical School. Only about 5 percent of the general, unhospitalized population carry C diff, and it usually does not cause health problems.
"We need to figure out ways to prevent patients from developing an infection when we give them tube feedings, antibiotics, proton pump inhibitors - all things which predispose people to getting an actual infection with C. diff that causes damage to the intestines or worse," said Young.
Now the researchers would like to apply computational tools like artificial intelligence predictions to identify those who are at risk of C. diff infections.
Sources: University of Michigan, Nature Medicine