New Model Teaches Us More About Why the Delta Variant is So Infectious
When the COVID-19 pandemic began to impact the world, researchers everywhere sprang into action. But studying an infectious virus like SARS-CoV-2 requires stringent safety protocols, special laboratories, properly trained and equipped staffers, and the right permits and models. Thus, many labs were limited and could only contribute so much to the effort to learn more about SARS-CoV-2. While those safety controls are absolutely necessary, it would also be good to find a way for more researchers to safely investigate the virus and the mutant forms that exist now, or could exist in the future.
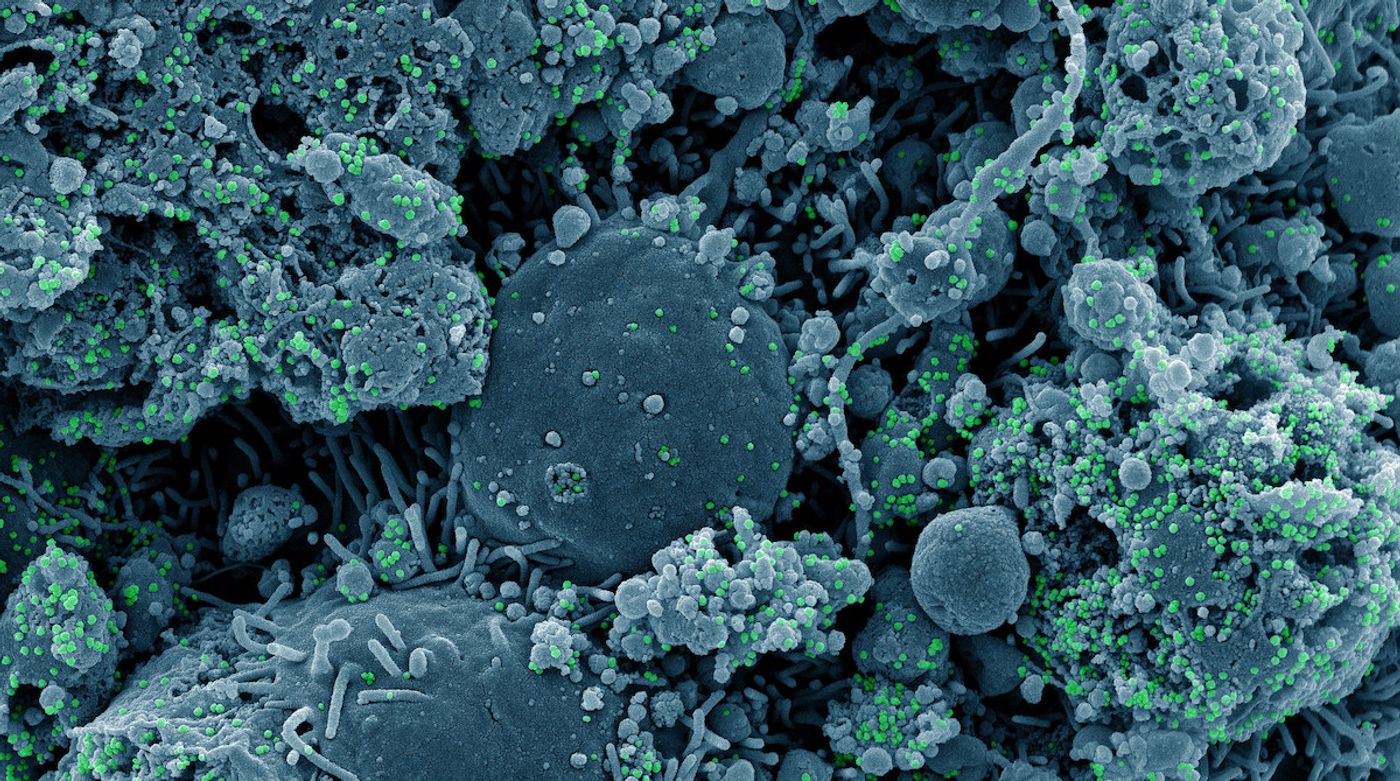
A team of researchers led by Professor Jennifer Doudna (one of the developers of the CRISPR gene-editing technology) has now done just that; they engineered virus-like particles (VLPs) that are made up of SARS-CoV-2 structural proteins, but they don't carry the viral genome. While VLPs are able to bind and infect cells in culture, they cannot release a viral genome inside a host cell to hijack the cellular machinery. The researchers shut down the ability of these VLPs to replicate or cause more infection.
In experiments using VLPs, the researchers added a messenger RNA molecule that would cause cells infected by the VLPs to glow. Next, they tried out various mutations on the viral proteins, one of which (R203M) is found in SARS-CoV-2 Delta, which is known to be more infectious than the original virus.
The researchers were surprised to find that when cells were infected with Delta VLPs, they glowed much more brightly.
“A single amino acid change found in Delta’s nucleocapsid protein supercharged the particles with ten times more mRNA compared with the original virus,” Doudna told Science. Cells that were infected by Alpha and Gamma VLPs glowed 7.5 and 4.2 times as much, respectively.
After this finding, the scientists turned back to the SARS-CoV-2 virus, under biosafety conditions. They found that a virus carrying a Delta (R203M) mutation generated 51 times more infectious virus particles in infected cells compared to cells infected by the original virus. In COVID-19 patients, these infectious particles are not always complete viruses, and those incomplete viral particles will not always be able to infect a cell. But if a virus is better at generating viral particles, more of the particles it makes may be infectious.
The study authors suggested that because SARS-CoV-2 Delta can produce more infectious particles, it can spread faster.
Hopefully, the system will teach us more about the virus, and how to stop the spread of COVID-19.
Sources: Science Magazine, Science