ALS Breakthrough: Two Targets Touted to Treat TDP-43 Trafficking Trouble
Researchers in the Ichida laboratory at the University of Southern California are dropping two papers this month set to redirect the search for amyotrophic lateral sclerosis (ALS) drug treatments.
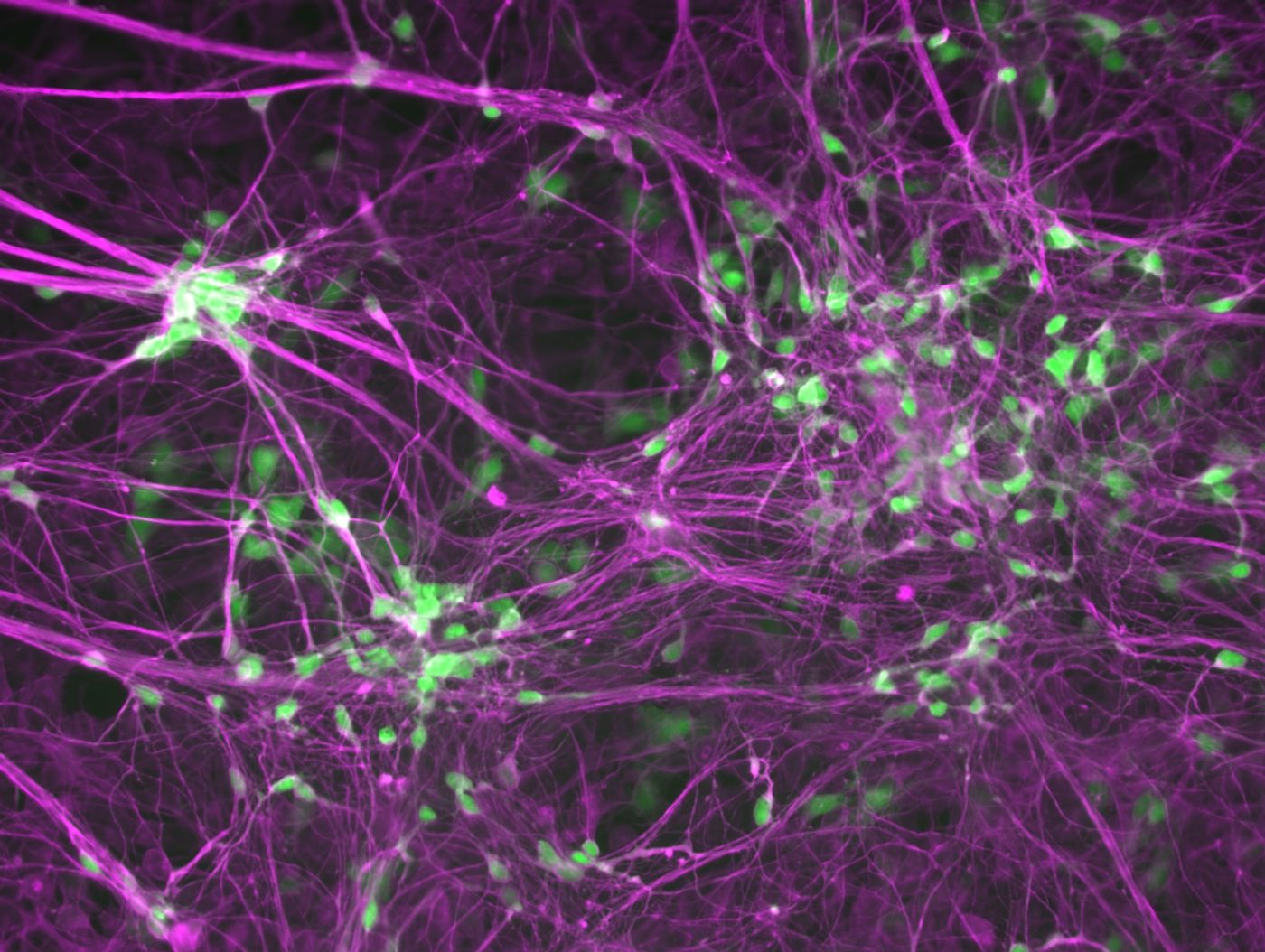
ALS, or Lou Gehrig’s disease, is a neurodegenerative disease with a diagnosis of two to five more years. Similar to Alzheimer’s disease, ALS is a proteinopathic disorder featuring the aggregation of pathological proteins, such as TDP-43, in neurons.
Ambitious researchers are attempting to rescue multiple forms of ALS with one treatment. As Gabriel Linares, a co-first author on both studies, explains, “a minority of patients have a variety of genetic causes of ALS that can be inherited within families, and a majority have what is known as ‘sporadic’ disease because its causes are unknown.” Linares describes the ultimate goal of developing “one treatment that will work for all patients with ALS.” The laboratory might have succeeded in not one but two moonshot treatments reported in Cell Stem Cell and good ol’ fashion Cell this month.
Researchers in the Ichida laboratory used model organisms and patient-derived motor neurons to screen various treatment approaches. They discovered two targets that, when suppressed, lead to better regulation of the ALS’s pathological proteins. Improved protein trafficking likely explains the decreased neuronal loss, improved behavior, and increased longevity of their model organisms.
In their Cell Stem Cell publication, the Ichida laboratory screened FDA-approved drugs and drug-like molecules to treat the two common forms of ALS. Several compounds that affect the signaling of the androgen hormone family popped up on their screens. Unfortunately, playing with hormones is a surefire way to generate undesired side effects.
The researchers looked for other ways to induce neurons whose transcriptional milieu resembles cells stimulated by androgen. Using a public bioinformatic database called Connectivity Map, developed by the Broad Institute of Harvard and MIT, the group identified the SYF2 gene.
Suppression of the SYF2 gene led to better TDP-43 protein management and reduced motor dysfunction in ALS model mice.
On the heels of their first publication, the Cell paper features these USC researchers inhibited the translation of an enzyme PIKFYVE kinase with antisense oligonucleotides and a drug called apilimod.
Inhibiting PIKFYVE kinase stimulated ALS-derived cells to increase their clearance of pathological proteins via specific types of exocytosis (amphisomes and multivesicular body). As Hung, the co-first author of the Cell paper, explains it, the laboratory was “able to pinpoint precisely how PIKFYVE inhibition mitigates neurodegeneration, which is important for informing the development of new targeted treatments,” said the co-first author of the Cell paper, Hung.
Increasing exocytosis via the suppression of SYF2 and PIKFYVE kinase led to healthier patient-derived ALS stem cells and model organisms. They offer targets that will work for both familial and de novo ALS.
Sources: Cell Stem Cell, and Cell