In a First, an mRNA Vaccine for a Deadly Bacterium is Created
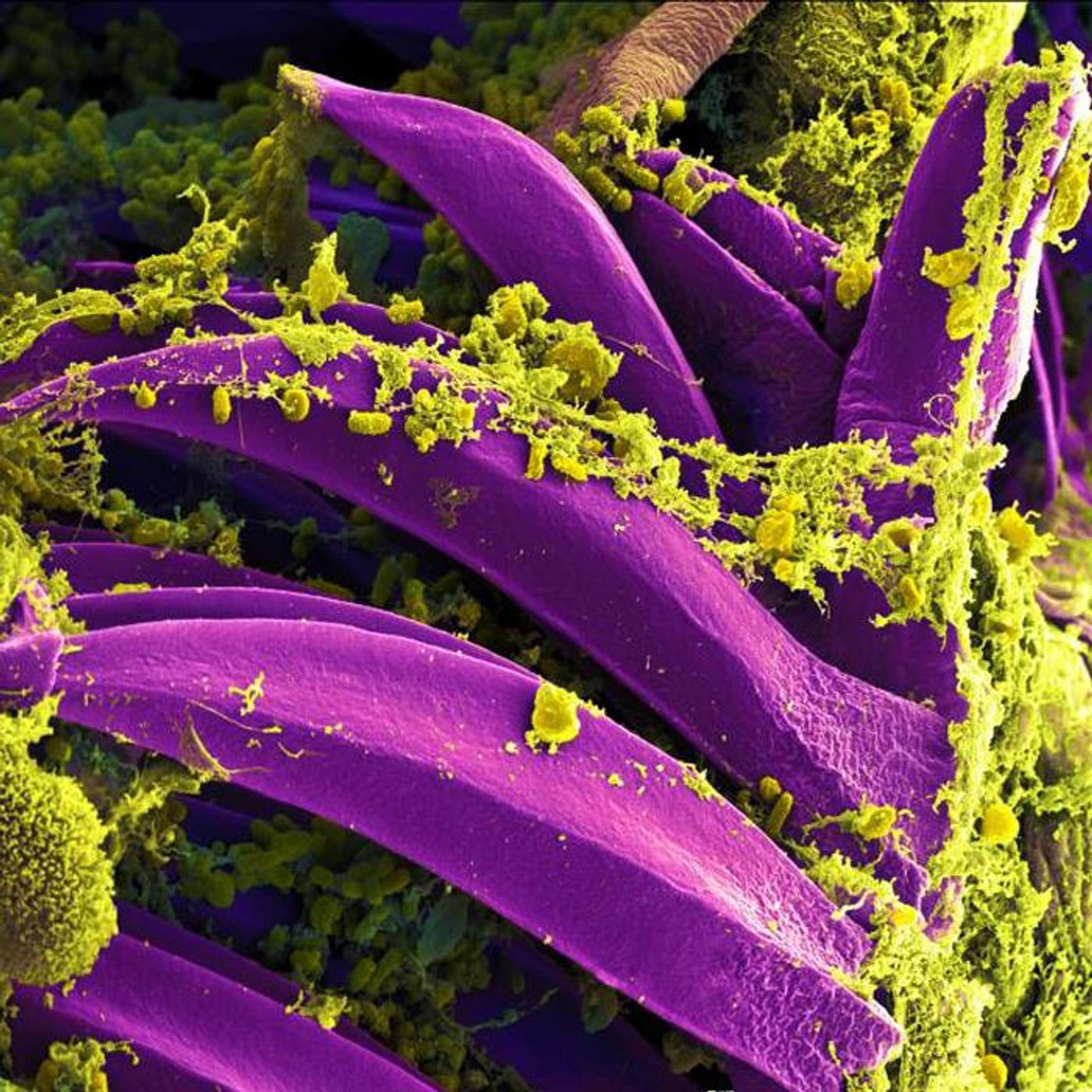
While the world became very familiar with mRNA vaccines because of the COVID-19 pandemic, mRNA vaccines have been around for awhile. Human clinical trials of mRNA vaccines first started in 2001, and by 2018, they were said to usher in a "new era in vaccinology." Now, scientists have engineered an mRNA vaccine against Yersinia pestis, which causes plague. Testing in an animal model indicated that the vaccine is totally effective. The researchers have suggested that this approach could be used to create vaccines for other microbial pathogens, including those that are antibiotic resistant. The findings have been reported in Science Advances.
One of the advantageous things about mRNA vaccines it that they can be developed very quickly compared to traditional vaccines. Only 63 days elapsed from the time researchers knew the SARS-CoV-2 genomic sequence until the first clinical trial for an mRNA-based COVID-19 vaccine, noted study co-leader Dr. Edo Kon of Tel Aviv University.
"However, until now scientists believed that mRNA vaccines against bacteria were biologically undoable. In our study we proved that it is, in fact, possible to develop 100 percent-effective mRNA vaccines for deadly bacteria," added Kon.
An mRNA vaccine against a virus utilizes portions of the viral genome. When a virus infects a host cell, it takes over the host cell machinery to produce viral proteins and more viral particles; viruses can't usually do this on their own. The mRNA in a vaccine and the corresponding viral proteins are very similar to what is actually used and made in host cells during an infection.
Bat bacterial cells don't need a host to make bacterial proteins or to replicate, noted Kon. "And since the evolutions of humans and bacteria are quite different from one another, proteins produced in bacteria can be different from those produced in human cells, even when based on the same genetic sequence.
While scientists have attempted to use human cells to generate bacterial proteins, this approach has not been successful in triggering antibody production, and has not stimulated immune protection. Although bacterial proteins are basically the same as ones that are made in the lab, these proteins undergo many modifications in human cells, such as the addition of sugar groups, when they are released from human cells, explained Kon.
In this work, the researchers made bacterial proteins while also bypassing the modifications. They enhanced the stability of the bacterial proteins so that they would not degrade rapidly in the human body by adding a portion of a human protein.
"The result was a significant immune response, with the immune system identifying the proteins in the vaccine as immunogenic bacterial proteins," said Kon. "By combining the two breakthrough strategies we obtained a full immune response."
Antibiotic resistance is a growing problem, and there few vaccines available for bacterial pathogens. This new approach could help us stave off the threat posed by antibiotic-resistant supergerms.
The vaccine was tested in an animal model that had been exposed to plague bacteria; all of the unvaccinated animals died, but the animals treated with the mRNA vaccine survived and did not get sick. A single dose was protective against infection within two weeks of administration, which could be a huge benefit if we are confronted with a bacterial pathogen that spreads rapidly. However, this vaccines, and others like it, still have to be tested for efficacy in humans. The COVID-19 pandemic also showed us that mRNA-based vaccines may not always stop infection, and pre-clinical models of the COVID-19 mRNA suggested that they were very protective in animals against SARS-CoV-2 infection.
Sources: Tel Aviv University, Science Advances