Novel 3D Bio-printed Leukemia Model Shows Potential for Treatment Testing Platform
Three-dimensional (3D) printing has become a common technique over the past two decades. Now, the technique has been adopted by the medical research field, in the form of 3D bioprinting, to enhance the development of life-saving treatments. Researchers from Italy developed a novel 3D bio-printed in vitro model for chronic lymphocytic leukemia (CLL). Their research was published online on May 3rd in the Frontiers in Immunology journal.
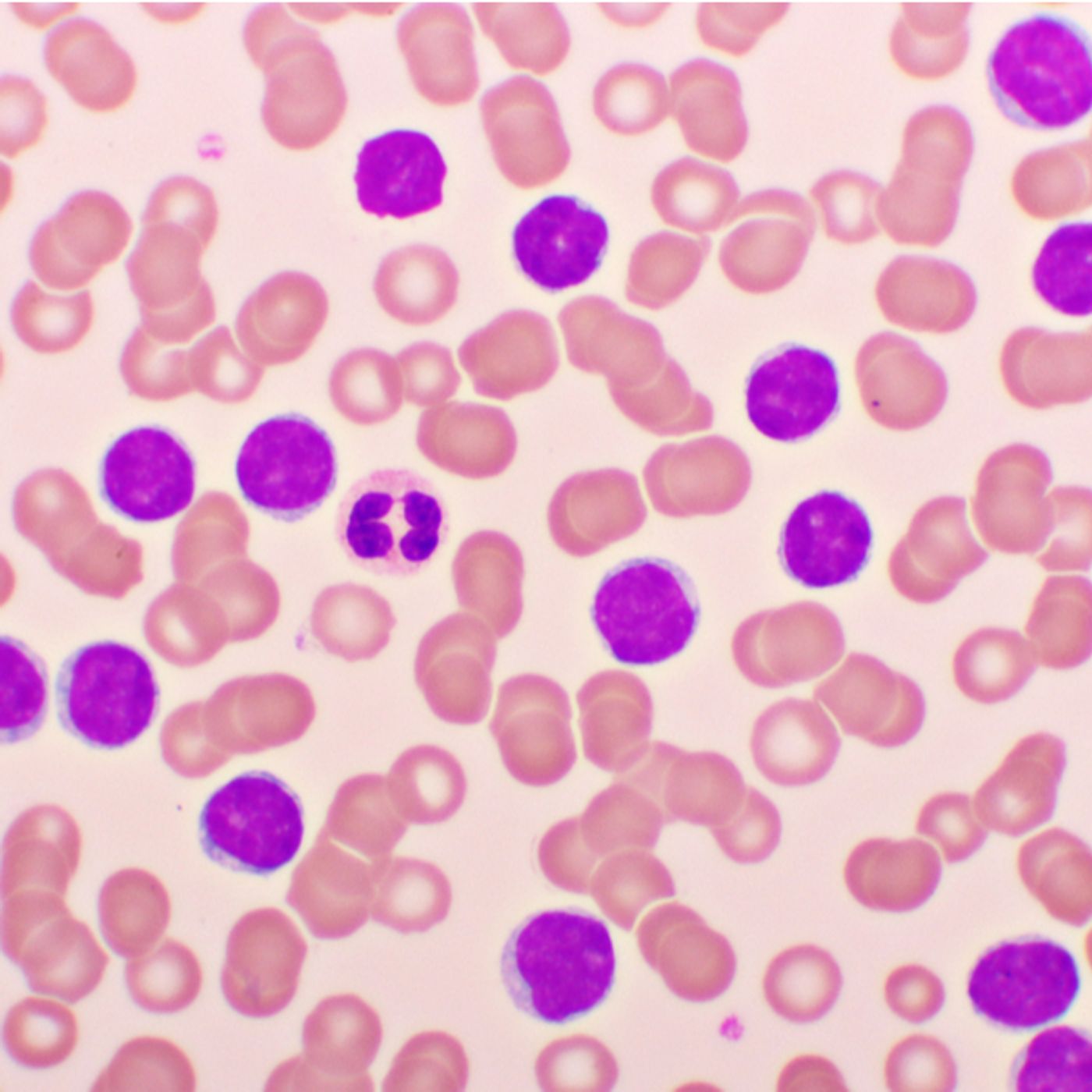
CLL is the most common leukemia in the western world. The disease impairs the immune system and leaves the patient at a high risk of succumbing to potentially deadly infections. Despite advances in research, CLL is incurable. CLL is characterized by the persistent accumulation of mature monoclonal B cells. B cells are a type of immune cell responsible for producing antibodies. However, in CLL, a genetic mutation causes one sub-type of B cell to over proliferate and they “clog” up the immune system in the peripheral blood, bone marrow, and secondary lymphoid (immune) tissues such as the spleen and lymph nodes.
The leukemia cells thrive in the immune microenvironments and scientists have not yet figured out how these cells organize and interact with the lymphoid tissues. Understanding these mechanisms is necessary to advance treatments. One of the challenges with studying CLL is that there were no good ways to look at the disease outside of a patient – until now.
Traditional cell culture is not a good way to study this disease, since leukemia cells do not live long in culture and the flat 2D cultures lack “cellular and spatial complexity”. However, bioprinting is a promising approach for generating complex and advanced 3D in vitro models. This method surrounds cells with a “bioink” that ideally mimics the extracellular matrix that the cells would be surrounded by the body. The encapsulated cells are then deposited in a layer-by-layer process defined by the researchers.
The Italian research team optimized the bioprinting method using cell lines, and then tested the method on primary cells which came from patients with CLL. During the cell culture, the team monitored CLL cell survival, gene expression, and phenotype, which showed that this model is a reproducible long-term 3D culture model for leukemia.
The outcomes from this research include:
1) The first successfully optimized bioprinting protocol for primary CLL cells;
2) Observation of the phenotypic and genetic differences between 2D and bioprinted 3D cultured CLL cells;
3) Successfully long-term culture achieved (up to 28 days); and
4) The culture system preserved the CLL cell phenotype, which will allow for more analysis.
This innovation is a novel tool that mimics the disease in a patient. This allows for a more reliable study of the molecular and cellular interactions that occur in CLL, and the researchers believe that it can also be used for clinical purposes to test individual patient responses to different cancer therapies. Other groups are successfully exploring this strategy for breast, brain, skin, and pancreatic cancers. Improved cancer models are a promising strategy for developing better cancer drugs, and appropriately matching them to patients.
Source: Frontiers in Immunology