Intestinal Macrophages Promote Chronic Inflammation in Obesity
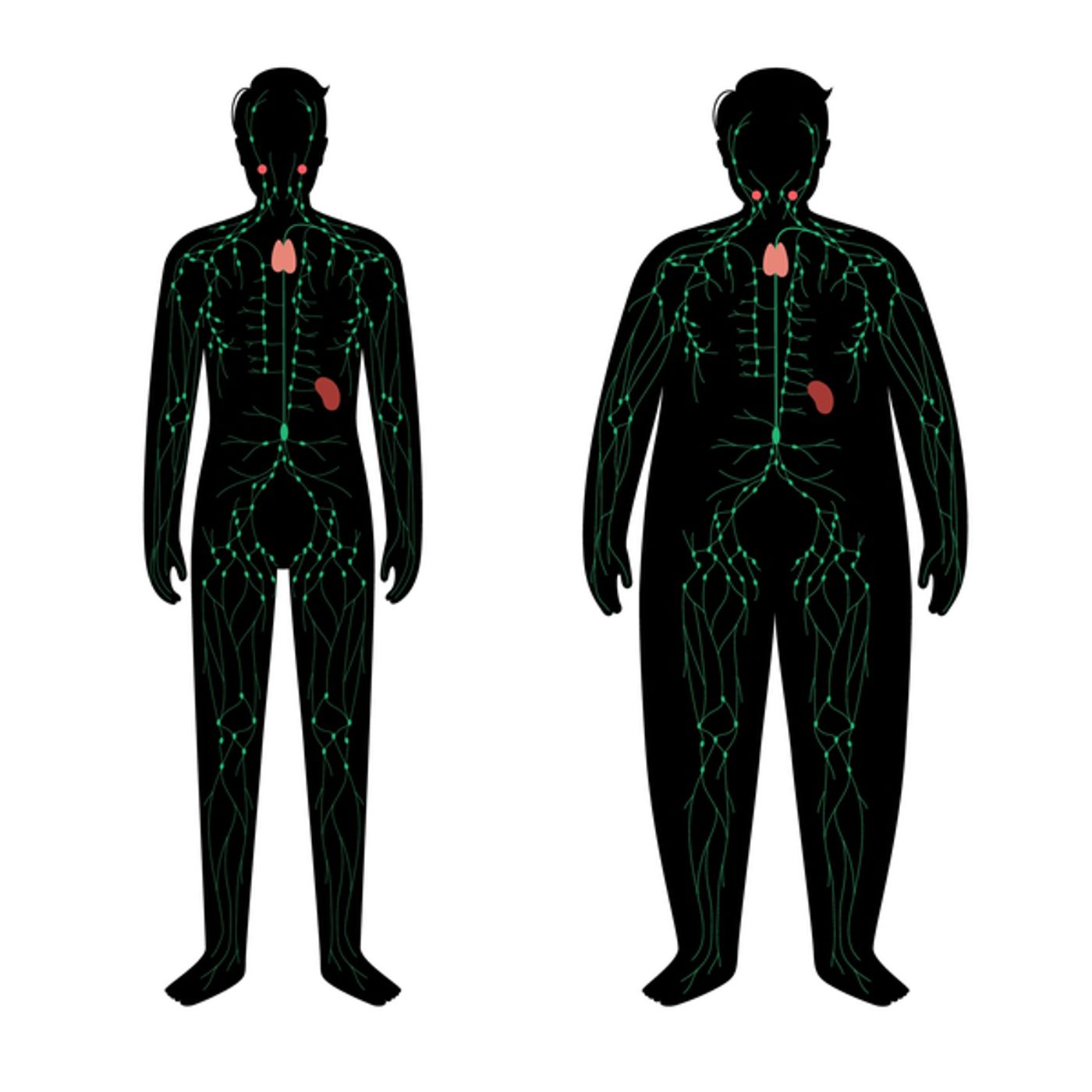
It is a well-known fact that obesity can lead to serious issues such as cardiovascular disease. This is partly due to the chronic low-grade inflammation that occurs in obese individuals. As scientists begin to understand what drives chronic inflammation in obesity, new treatment targets for metabolic diseases may be found.
A research group from Switzerland hypothesized that immune cells in the gut (gastrointestinal tract) must trigger chronic inflammation in obese individuals. Their discovery and characterization of the gut immune cells in obese versus non-obese individuals was published in early May in Frontiers Immunology.
The immune system in our gut is unique because it is constantly exposed to food, bacteria (microbiota), and metabolites. Immune cells are a vital part of the intestinal mucosa that form a barrier between the foreign products in our gut and the rest of our body. Monocytes are a type of innate immune cell in the blood, and they change into macrophages once they enter the gut tissues. Macrophages are the most common immune cell in a healthy gut.
The researchers characterized human intestinal macrophages in non-obese and obese individuals at different locations along the GI tract, since potential differences were not known before this study. The team also looked at how body composition, different lifestyle behaviors (nutrition and physical activity), and disease variables impacted innate immunity in the gut.
This study was a prospective, single-center observational study that enrolled 54 subjects. Obesity was determined based on the participants' body mass index (BMI). Biopsies were taken from obese and non-obese individuals during routine scheduled procedures such as screening colonoscopies, gastroscopy, or bariatric surgery. The immune cells were isolated from the biopsied tissues and flow cytometry was used to identify the immune cell sub-populations.
There is a delicate balance between the immune cell sub-populations: imbalance can lead to disease. In a healthy gut, most of the intestinal macrophages are more mature anti-inflammatory macrophages. Previous research has shown that in IBD, macrophages retain their immature pro-inflammatory phenotype, which drives the disease.
The research team identified five distinct macrophage subpopulations in the GI tract and three blood monocyte subpopulations. The monocyte subpopulations were present in both obese and non-obese individuals, and they replenish the intestinal macrophages.
However, obese individuals had more pro-inflammatory macrophages throughout their GI tract and they also had more intermediate blood monocytes. Additionally, the pro-inflammatory macrophage subpopulation P2 and the number of intermediate blood monocytes correlated with body weight and unhealthy lifestyle habits.
This data reveals a potential link between unhealthy lifestyle behaviors and changes in gut innate immunity. Since a role for the mucosal innate immune system in obese individuals is established, these biological mechanisms may be exploited to find new treatments for metabolic disorders such as obesity. Future studies, such as what triggers more pro-inflammatory macrophages in obesity, are necessary to fully complete the picture.
Source: Frontiers Immunology