Solving the Mystery of Failed Staph Vaccines Shows How to Make Them Effective
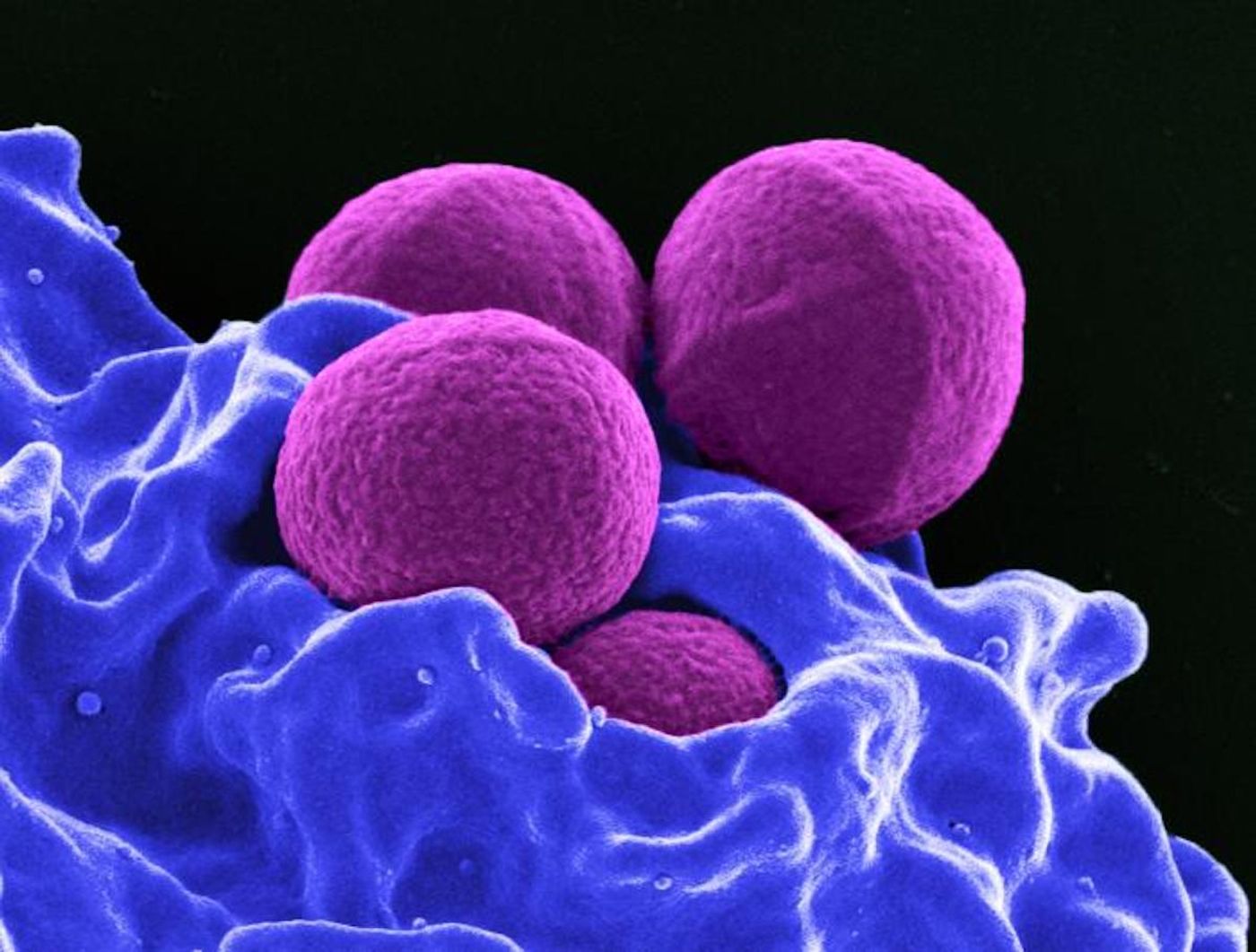
Some common bacteria like Staphylococcus aureus have both harmless and pathogenic versions. While staph is often harmless, it can also cause food poisoning or infect people as MRSA, (methicillin-resistant S. aureus), which can cause fatal illnesses. Antibiotic-resistant bacteria are considered to pose a serious threat to public health, and MRSA is one of the main culprits right now. As such, researchers have tried to develop a vaccine that prevents serious staph infection. But so far, every vaccine candidate has failed in human trials. Now, scientists have learned why. The findings have been reported in Cell Host & Microbe.
People are exposed to staph microbes soon after birth, because the bacteria are everywhere. About half of all babies host colonies of Staphylococcus aureus within two months of birth, and most have also generated antibodies that can stave off a staph infection. However, mouse models that have been used to test staph vaccines have not typically been espoused to S. aureus; they are kept in cleaner environments. Therefore, the researchers hypothesized that lab mice with no previous staph exposure were responding well to vaccines, while humans that have been exposed to staph and have their own immunity do not react to the same vaccines with infection-preventing antibodies.
"It's a longstanding and one of the most enigmatic issues of the staphylococcal field. None of these human trials have worked and scientists have struggled to find a reason," said George Liu, MD, Ph.D., a professor of pediatrics at University of California San Diego School, among other appointments.
"Staph vaccines appear so easy to make in laboratory mice because they rarely see S. aureus, but humans are exposed to staph beginning in the first weeks of life and, in order to coexist, staph appears to have developed many strategies to render ineffective our immune response against them," explained first study author and project scientist Chih-Ming Tsai, Ph.D.
In this study, the researchers tested their hypothesis by simulating a failed trial. A previously developed staph vaccine was designed to target a protein called IsdB that aids in the uptake of iron, which is essential to the microbe.
When mice that had not been exposed to staph were given the vaccine, it led to the production of antibodies against the entire IsdB protein, and the antibodies were protective; they disrupted staph microbes. But when mice had been exposed to staph before they got the vaccine, they did not generate antibodies that prevented disease, and only generated non-protective antibodies. Booster shots did not improve the situation, and only led to the production of more ineffective antibodies.
Next, the scientists combined human antibodies against IsdB with protective antibodies that were generated after a vaccine treatment.
"We surmised that if we could vaccinate only against the protective component of IsdB, we might be able to prevent suppression by bad immune response memory," said Tsai.
Indeed, the researchers were able to vaccinate mice against a protective portion of the IsdB protein. Then, mice were protected from infection by the vaccine even when they'd already been exposed to staph.
Liu noted that a faulty memory of a pathogen and the immune response that goes along with it could explain why human trials have failed.
"It is even possible that the same principle might also explain why many other hard-to-make vaccines have failed. If we are proven correct, an effective staph vaccine may not be too far away," said Liu.
Sources: University of California - San Diego, Cell Host & Microbe