A Dietary Fiber Can Affect the Microbiome & Trigger Inflammation
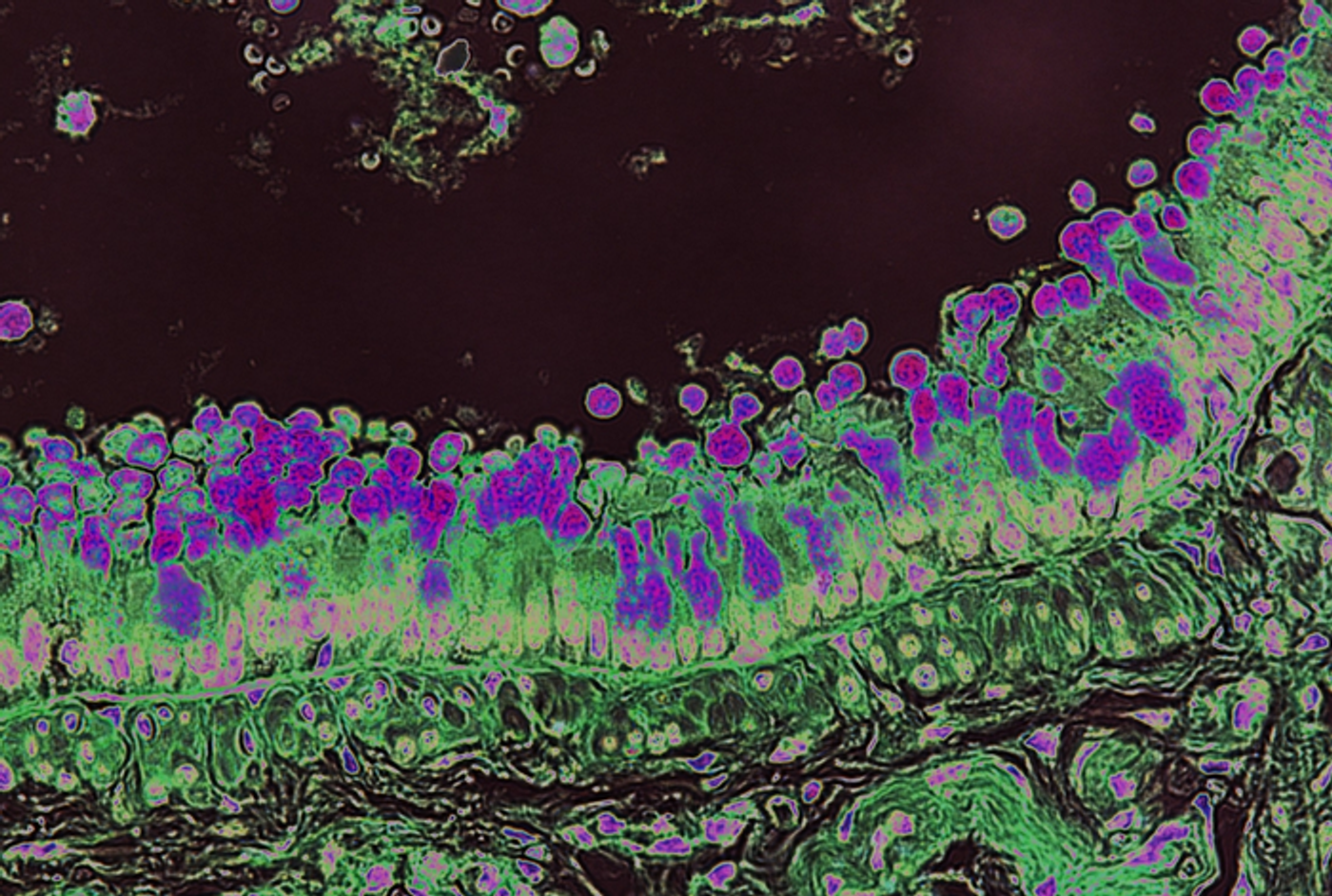
Inulin is one type of fiber that we consume in our diets, and it can be found in fruits, vegetables, and grains including wheat, asparagus, bananas, garlic, and onions. It's also commonly used in health supplements. New research has shown that inulin can trigger inflammation in the gut and other parts of the body that is related to an allergic reaction. Dietary inulin appears to change the metabolism of gut microbes, which leads to a phenomenon known as type 2 inflammation in the lungs and gut. But inulin can have some good effects on immunity as well. The findings have been reported in Nature.
Type 2 inflammation involves a subset of CD4+ T cells called Th2 cells, which release certain inflammatory signals known as cytokines. Type 2 inflammation is typically thought of as a defense against parasites, and plays a role in healing when it is working correctly. But disruption in type 2 inflammatory pathways are thought to be related to inflammatory disorders including asthma and allergies.
Previous research has shown that inulin can act as a probiotic that promotes the growth of healthy gut bacteria, leading to higher levels of anti-inflammatory regulatory T cells (Tregs).
In this work, the investigators used a mouse model; there were two groups, one of which was given a high-inulin diet for two weeks while the other ate normal chow. The researchers found that the high-inulin diet did increase the number of Tregs, while also triggering increases in the levels of white blood cells called eosinophils in the gut and lungs. High levels of eosinophils are considered a hallmark of type 2 inflammation, and is often observed in cases of asthma and seasonal allergies.
A type of gut bacteria known as Bacteroidetes can be found in both mice and humans, and these bacteria express an enzyme that metabolizes bile acids. Inulin boosts the growth of Bacteroidetes, which elevates bile acid levels. The researchers determined that bile acids in the blood affect immune cells called group 2 innate lymphoid cells (ILC2s), which impact the eosinophil response.
"We were amazed to find such a strong association between inulin supplementation and increased bile acid levels," said co-corresponding study author Dr. Frank Schroeder, a professor at Cornell University's Ithaca campus.
When mice that lack gut microbes were colonized with Bacteroidetes that lacked a bile acid-producing gene, the pathway was blocked and the allergic inflammation was halted.
The study authors noted, however, that inulin is not a bad fiber simply because it has been linked to an increase in type 2 inflammation. Although inulin exacerbated type 2 airway inflammation caused by allergens in a mouse model, inulin was also confirmed to increase Treg levels, which can counter inflammation. The type 2 immune response, which increase mucus production in the guts and lungs, is not necessarily problematic for healthy people.
Now the researchers want to investigate other dietary fibers and dietary supplements to examine how they impact immunity, health, and disease.
Sources: Weill Cornell Medical College, Nature