Discovery Changes What We Knew About B Cell Activation
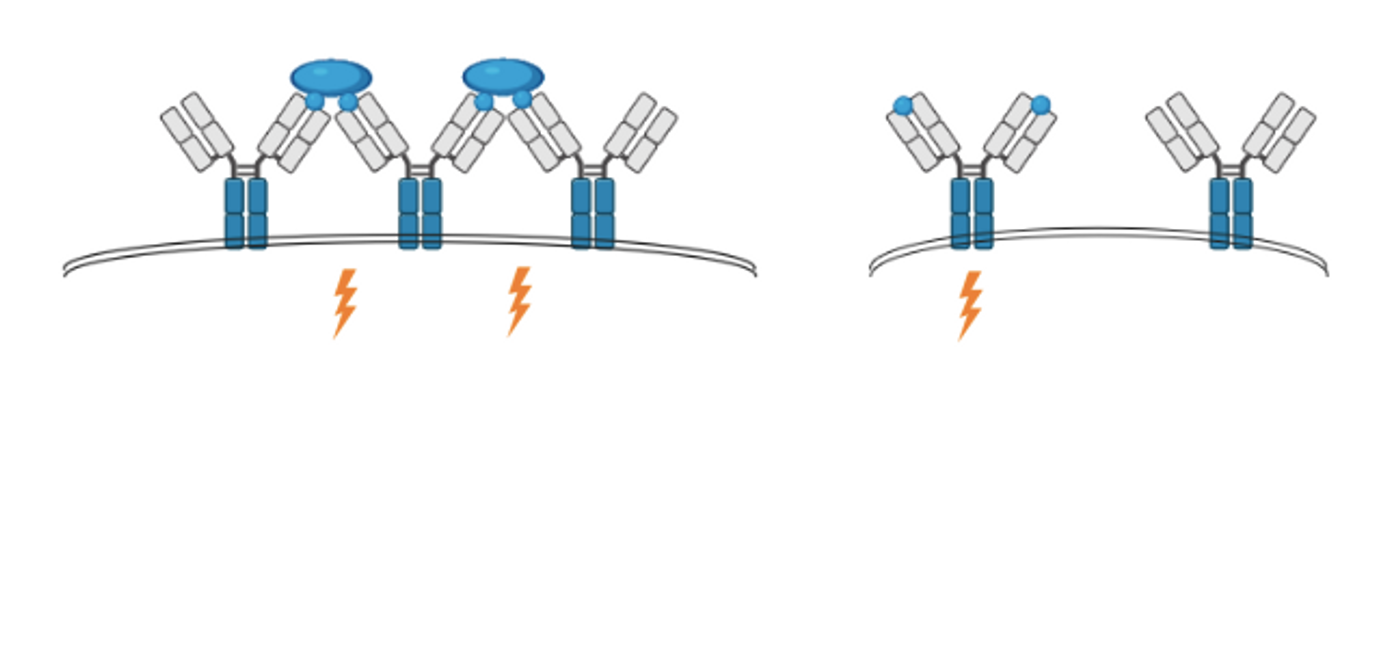
It has been thought that in the first step in B cell activation, when these immune cells recognize an infectious pathogen, an antigen from that pathogen had to bind to multiple receptors on the surface of B cells. But this textbook information may have to be changed. New research has shown that individual antigens from pathogens that bind a single B receptor at a time can also activate the B cells. These findings have been reported in Nature Communications.
B cell receptors were thought to be composed of a membrane-bound immunoglobulin (mIg) and two transmembrane proteins: Igα and Igβ. When an antigen from a pathogen binds to the BCR, a cascade of signals is unleashed, which leads to the proliferation of B cells, antibody production, and the creation of memory B cells that can respond to a similar infection later. When we receive a vaccine or when we get an infection, this is how B cells produce crucial antibodies that can neutralize infections. While the signaling cascade that leads to these outcomes is well-understood, the earliest steps of BCR activation have not been clear.
B cells may also generate dangerous antibodies that can cause autoimmunity or allergies, and this work may lead to new insights about how or why that occurs.
"The result is significant because it represents a breakthrough in our understanding of how these important immune cells recognize their enemies. Once we understand what is going on, we can imitate it in the design of new vaccines, to ensure maximum effect," noted senior study author Søren Degn, an associate professor at Aarhus University.
The study has offered an alternative to theories and observations about BCR activation that have been conflicting or incomplete; the prevailing hypothesis has not been able to explain all of the data, noted the study authors.
This work could also help scientists who design vaccines do a better job of mimicking pathogens to trigger a powerful immune response after vaccination, noted Degn.
A technique called DNA-Paint super-resolution microscopy was used in this study, and is outlined in the following video.
The study authors have also initiated preclinical studies to see whether these findings will improve the design and efficacy of vaccines. They also want to learn more about how to reverse this process and halt harmful immune responses like those seen in autoimmunity and allergy, although that investigation will take longer.
"We have shown that the way in which the activation of B cells has been explained over the past thirty or forty years is wrong. This is an important finding, because it opens the door to better vaccines and better treatment of a large group of diseases," added Degn.
Sources: Aarhus University, Nature Communications