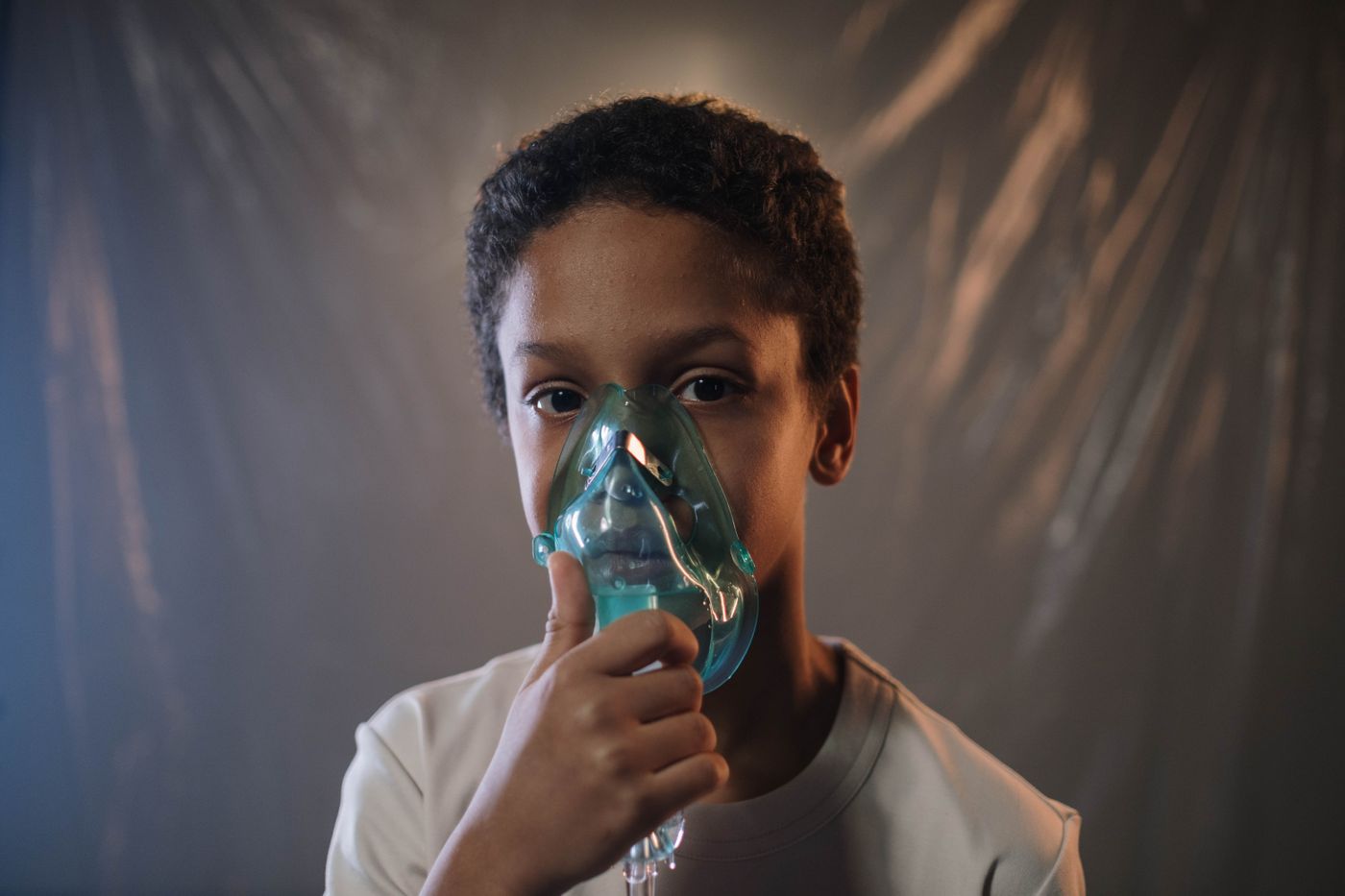Over Sanitation Not Responsible for Heightened Allergies, Research Suggests
In the 20th century, the rise in allergic diseases baffled researchers. Asthma rates surged twelvefold in numerous developed countries from a mere 0.29% in 1966 to 3.5% in 2003. While genetics play a role, the lion's share of blame often falls on shifts in modern diets, improved sanitation, vaccinations, and easy access to antibiotics.
This sets the stage for the "hygiene hypothesis," suggesting that our modern, overly sanitized environment is causing our immune systems to overreact to benign triggers. Yet, there's a compelling link between a richer gut microbiome diversity and a lower incidence of allergic diseases.
The microbiome comprises trillions of bacteria, viruses, and fungi, presenting a complexity that is impossible to standardize in a laboratory setting. Moreover, researchers cannot simply order an identical pathogen exposure kit for all their animal subjects. These limitations highlight why the conventional laboratory mouse, bred under pathogen-free conditions, falls short of fully replicating human immune responses.
Enter the 'wildling' mice, a specially developed breed created by Dr Stephan Rosshart at the Karolinska Institutet of Sweden to bridge this gap. Wildlings, carrying diverse microbiomes from surrogate wild mouse mothers, have shown promise in mimicking human immune responses, paving the way for a new groundbreaking study by Junjie Ma, Rosshart, and colleagues.
Their study, published in Science Immunology, aimed to unravel the impact of early-life microbial exposures on life-long allergic immune responses by comparing wildling mice to standard laboratory mice. The mice were exposed to allergens, including the ubiquitously allergic house dust mites (HDM), fungi associated with hay fever, and other common triggers for allergic reactions.
Surprisingly, just like laboratory mice, wildling mice exhibited robust immune responses to real-world pathogen exposure despite their rich microbiomes. Wildlings even displayed heightened reactivity to HDM.
This challenges the assumption that early-life microbial exposure can effectively suppress allergic sensitization and inflammation. The implications are profound, suggesting that altering early-life environments is not the key to prevent allergies. For the approximately 300 million worldwide affected by bronchial asthma, this prompts a reevaluation of our approach to finding cures beyond symptom control.
“Our study may help to recalibrate scientists' view on the hygiene hypothesis,” explains Stephan Rosshart, an author of the paper (via EurekAlert!). While current treatments like anti-immunoglobulin E can mitigate symptoms, a quest for more definitive, corrective cures is urgent. The study encourages researchers to widen their scope beyond the hygiene hypothesis, investigating varied factors influencing the development of allergic diseases. Rosshart stresses the importance of researchers in the field taking “a closer look at other factors such as indoor living, physical activity, pollutants, and chemical compounds present in the modern world.” As this medical mystery unfolds, it prompts a return to the white board for new conversation about strategies to combat this growing epidemic of allergic diseases.
Sources: Science Immunology, Science, Nutrients, Nature Signal Transduction and Targeted Therapy, EurekAlert!